Rebecca Aburn
So, one of your patients has made a complaint about the service they have received at your clinic. It’s not what you had planned, right? You’re doing all you can to improve their quality of life … so, what went wrong? And how can you make sure it doesn’t happen again?
A diabetic foot clinic in New Zealand experienced a complaint from one of their patients, and as a consequence has analyzed the issues and worked hard with their patients to develop a co-designed healthcare approach that puts their patients in the center of the care team.
What went wrong?
After analyzing the complaint, engaging patients and proactively getting feedback, giving the health professionals the opportunity to share their experiences and discuss ideas about what worked and what didn’t, it became clear why there had been a complaint.
There was poor communication between the health professionals, a lack of a clear care plan, and many different ways of caring for the patient by different health professionals, as well as inconsistent documentation of the care and healing progress.
The way forward
Improving patient engagement for not just the one patient who complained but all of the patients in the clinic became a central focus for the whole team. The clinic developed a co-design method to improve their delivery of care by: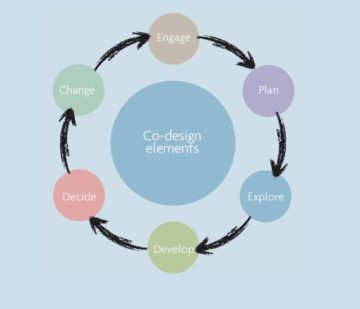
- Encouraging patients to have an equal role in the review and development of the care provided
- Improving communication, documentation, and care planning
- Designing their services around patient experiences
- Using tools, such as experience-based surveys, to gather feedback and develop their services to better meets the needs of their patients
The importance of accurate information
For the care team to provide accurate information to their patients, they needed to have a system that would provide accurate wound assessment information they could rely on. The diabetic foot clinic used the Silhouette system to help them audit their practices with 30 patients. The data they collected with Silhouette formed the basis for their care plan, enabled them to document healing progress and identify barriers to healing.
Their audit revealed that patient inclusion in tracking their healing empowered and motivated them to participate in their treatment plan.
Some of the patient comments included:
“I love being able to see the progress”
“It gave me hope”
“The graph and the photos it proves it”
“I knew when I was doing too much – the picture does not lie”
“Has helped me to manage my wound better and gain control”
Successful outcomes
Placing the patient in the center of the care team and engaging them in their own healing journey was key to this clinic’s success. So too was having the Silhouette platform to enable accurate wound assessments that encouraged patient engagement and affirmed their progress towards their goals. Being able to monitor the patients between treatments, their wound healing progress, and other factors has also enabled clinicians to predict healing peaks and troughs.