How to improve wound assessment performance
Reliable, productive wound assessment processes
The practitioner’s wound assessment is a basic component of wound care. At the point-of-care, at discrete moments in time, a practitioner – often without specialized knowledge of wounds – inspects, measures, images, and documents each of the patient’s wounds. Despite all their time and efforts, traditional methods can lead to questionable accuracy, inconsistent quality, and poor compliance with documentation standards.
Over time, many practitioners make many assessments under these conditions, thus accumulating a generally unreliable body of information.

Silhouette is a non-invasive wound surveillance system that supports the achievement of better patient outcomes.
Why is wound assessment so important?
The most fundamental and often quoted metric for measuring and reporting wound healing progress is that of area reduction over time. Because this metric is used for basic evaluation of a wound’s progress (1), it is frequently used to evaluate the effectiveness of wound care processes and practices and is becoming an important determinant of reimbursement.
In general clinical practice today, traditional wound measurement techniques are cumbersome and inaccurate – introducing errors of as much as 40% (2). As the focus on managing health care costs continues to intensify, such imprecision is exposing healthcare organizations to risks and adverse financial consequences. For instance, inaccurate measurements may undermine confidence in use of debridement or advanced therapies, or bring into question the adequacy of documentation and evidence of the status of a wound during a transfer between care settings.
Did you know that Silhouette measures the percentage of change in wound size between assessments?
Wound surveillance: How Silhouette works
Wound surveillance is the ongoing and systematic collection, analysis and dissemination of accurate data about wound behavior to improve healing outcomes. However, without accurate tools, effective wound surveillance is difficult.
The Silhouette system offers a way to systematically and easily collect accurate wound data. Silhouette is a 3D measurement, imaging and documentation system that provides precise measurement and healing trends along with comprehensive wound surveillance support.
The Silhouette® system is made up of three main parts – a point of care imaging device, smart software and a wound information database:
- The SilhouetteStar™ specialized camera (pictured right) captures the wound image;
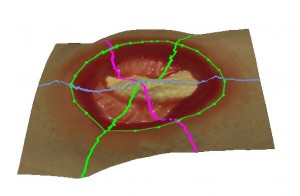
- SilhouetteConnect™ software creates a 3D model of the wound based on the data acquired by SilhouetteStar (see below), derives measurements from the model, and records standardized notes;
- SilhouetteCentral™, a secure Internet-accessible database that stores and consolidates the information obtained from the organization’s SilhouetteStar + SilhouetteConnect devices, sharing data with EHRs such as Epic, Meditech, Cerner, and CPRS/VistA, Concerto, and PIMSY.
Accurate measurement and precise healing trends
Silhouette enables clinicians to capture accurate and precise measurements and derive reliable healing trends. A recent study found that any single Silhouette-derived measurement is likely to be within approximately 2% for area, 1% for perimeter, 5% for average depth and 5% for volume (95% confidence interval). Inter- and intra-rater variability is extremely low – <1% for area and perimeter, and <2% for average depth and volume. This indicates that repeated measurements over time – even by different assessors – will detect small differences as a wound changes in size and dimensions. The healing trends presented are statistically meaningful and clinically useful.
This accuracy level, made possible by 3D laser technology, means Silhouette can help practitioners to detect small changes in wound size immediately, leading to earlier intervention, higher quality evidence, and better-informed decision-making.
Wound surveillance is the ongoing and systematic collection, analysis and dissemination of accurate data about wound behavior to improve healing outcomes.
Wound imaging
Silhouette addresses typical wound image management issues, producing high quality images at the point-of-care. The SilhouetteStar device has no user-adjustable settings – the camera has its own light source, and the laser lines position the camera for optimum focus and composition. There is only one moving part – the button which captures the wound image.
Silhouette assessments are recorded directly into the patient record. Images are not stored on the camera because image data is transferred in real-time to the SilhouetteConnect software. The wound photographs and measurement information are displayed together so the practitioner, or any authorized stakeholder logged in remotely, can compare the image with healing trends and other clinical information.
Documentation
 Silhouette provides reliable documentation for reimbursement, defense and audit purposes. At the point of care, customized wound notes fields in Silhouette enable practitioners to record standardized and free text documentation about the wound and the patient. These are exported into Wound Assessment Reports combining measurements, graphs displaying the latest healing trends, images, and documentation. Upon synchronization, this data is transferred to SilhouetteCentral via an Internet connection, enabling other authorized stakeholders to view the assessment information. Here, reports can be generated based on aggregated patient data. Using this facility, clinical managers can, for instance, track whether assessments are occurring as often as required, identify outliers and review wound outcomes metrics. If SilhouetteCentral is integrated with the EMR, the wound information can also be transferred to this system.
Silhouette provides reliable documentation for reimbursement, defense and audit purposes. At the point of care, customized wound notes fields in Silhouette enable practitioners to record standardized and free text documentation about the wound and the patient. These are exported into Wound Assessment Reports combining measurements, graphs displaying the latest healing trends, images, and documentation. Upon synchronization, this data is transferred to SilhouetteCentral via an Internet connection, enabling other authorized stakeholders to view the assessment information. Here, reports can be generated based on aggregated patient data. Using this facility, clinical managers can, for instance, track whether assessments are occurring as often as required, identify outliers and review wound outcomes metrics. If SilhouetteCentral is integrated with the EMR, the wound information can also be transferred to this system.
Process improvement
Silhouette addresses common process-related challenges associated with managing wound assessment.
- With Silhouette, communication improves because all stakeholders can monitor wound assessments and healing trends remotely, review the images and measurements of the wound, review the assessment practice of others, and obtain second opinions and consensus on diagnosis and treatment decisions.
- Wound specialists can extend their reach using Silhouette, as it enables them to gather the information they need from non-specialists at the point-of-care, supervise and review these assessments, and focus their efforts on outliers and urgent cases. Wound specialists can improve the assessment capability of non-specialists using Silhouette information for feedback and training.
- Silhouette has the ability to record wound treatment decisions and link this information to wound stage and healing progress. This means facilities can monitor the relationship between treatments, wound healing progress and other factors, and clinicians can justify the use of more expensive treatments if necessary.
- Silhouette gives organizations oversight of the entire wound care effort. They can choose how prescriptive their Silhouette assessment processes will be. If strict protocols are required, Silhouette offers a “protocol engine” with a built-in structured workflow.
- If there is an adverse event such as a suspected hospital-acquired pressure ulcer, the whole “story” of the wound is provided in one place, avoiding the scramble for piecemeal documentation when a particular wound outcome is under scrutiny.
Silhouette makes our jobs easier in assessing wound progress and treatment planning. Patients can see progress and understand the interventions we are using and – importantly – their own role in reaching treatment goals.
– Maureen Bates, Podiatry Manager at Diabetic Foot Clinic Team at Kings College Hospital NHS Foundation Trust, London, UK
Privacy, safety, data security and compliance
Silhouette mitigates risks associated with the handling of patient information.
Because images and wound assessment information are recorded directly in the patient record, the risk of error is minimized. Silhouette also supports a variety of protocols and functionality, including HL7 patient demographic information exchange, DICOM image transfer, and DICOM Encapsulated PDF report creation and transfer. Silhouette is designed to support PHI, HIPAA and Health Information Technology for Economic and Clinical Health Act (HITECH) compliance.
The Silhouette system is compliant with all major accreditation marks. Regulatory clearance includes an FDA Class 1 approval (US), along with CE Mark (Europe), Health Canada – Therapeutic Products Directorate (Canada), TGA approval (Australia), Health Services Authority (Singapore) and WAND registration (New Zealand).
Read more about Silhouette accuracy and precision.
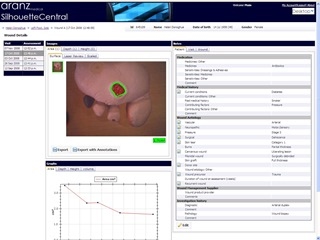
SilhouetteCentral Wound Details screen
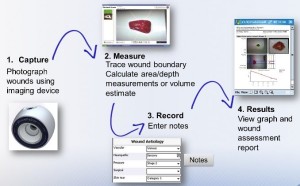
Silhouette streamlines wound assessment processes, leading to greater efficiencies, reduced risk and cost, and better wound outcomes
References